Key Takeaways
- Weight-loss drugs are being rolled out in a controlled manner by the NHS to help manage obesity for Brits most in need. However, the ballooning private market is raising health concerns and widening health inequalities.
- Medical research points to the regaining of weight after cessation of weight loss drugs. This isn’t cost-effective and poses a threat to the NHS if not properly monitored.
- The growth of Glucagon-like peptide-1 (GLP-1) medication provides economic opportunities that include greater labour force participation, job creation and investment into the UK life sciences sector. If paired with tighter regulation, weight-loss drugs could help drive lasting, positive change across the food industry.
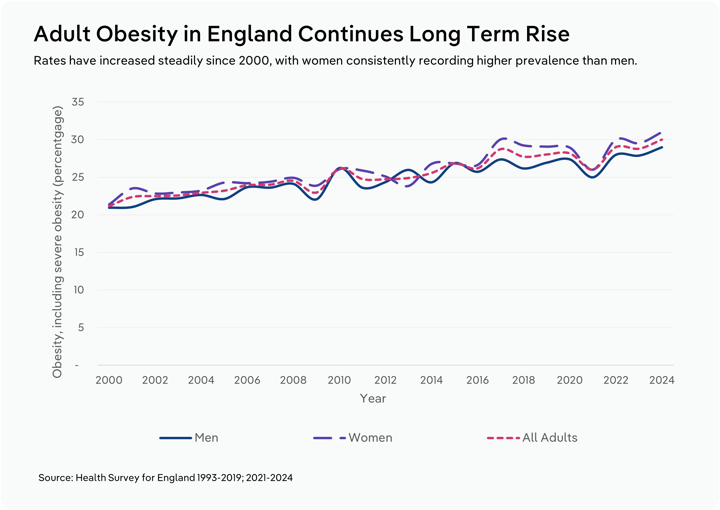
The World Health Organisation defines obesity in adults as a Body Mass Index (BMI) greater than or equal to 30. Hybrid working environments are encouraging more sedentary lifestyles among many Brits, contributing to rising obesity rates. The Health Survey for England found that 30% of adults were living with obesity in 2024. This marks an increase from the approximately 25% of adults reported as obese in 2014.
The popularity of weight-loss drugs as a route to tackle obesity is swelling, reflecting a growing preference for rapid, medication-based solutions. An estimated 1.6 million adults in England, Wales and Scotland used weight loss drugs like Wegovy and Mounjaro to help lose weight between 2024 and 2025. UCL’s research, conducted in early 2025, also found that an additional 3.3 million people said they were interested in using weight-loss drugs over the next year.
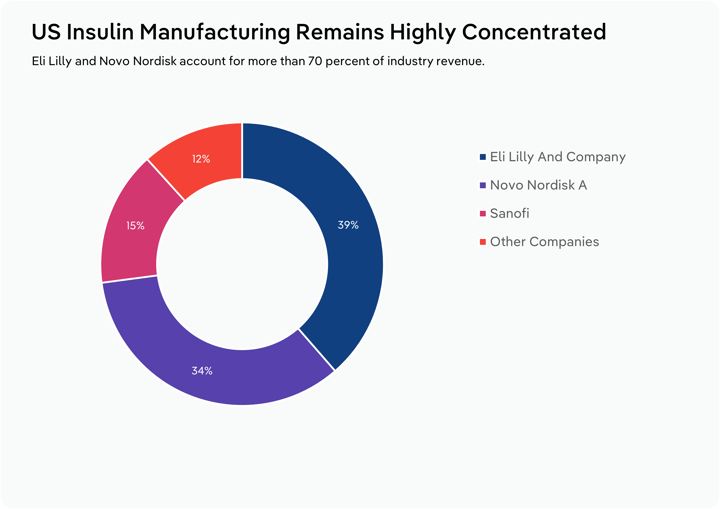
The weight-loss drug market is dominated by US company Eli Lily, whose stock has climbed 36% in 2025, signalling investor confidence in the company’s prospects and in the growth potential of weight-loss and wider pharmaceutical markets and Novo Nordisk (a Danish company). Eli Lily makes tirzepatide, sold as Mounjaro, for weight loss and Novo Nordisk makes semaglutide, sold as Ozempic, for diabetes and Wegovy for weight loss. Originally, Glucagon-like peptide-1 (GLP-1) was used only for the treatment of Type 2 diabetes, but after clinical trials showed significant signs of weight loss, semaglutide and tirzepatide were approved for weight loss by the National Institute for Health and Care Excellence (NICE) in October 2023. GLP-1 receptor agonists like semaglutide and tirzepatide help by increasing insulin secretion after eating meals, lowering blood sugar levels and intensifying the feeling of fullness, thereby suppressing appetite. However, people taking GLP-1 receptor agonists are also at heightened risk of developing drug-induced acute pancreatitis, nausea, vomiting, arthritis and low blood pressure.
What weight-loss jabs mean for the NHS
Obesity costs the NHS over £11.4 billion every year, with wider societal costs of approximately £74.3 billion driven by ill health that sidelines people from work and drags down productivity. Hospitals in the UK, especially the NHS, are currently struggling under extensive waiting lists and staff shortages. The NHS England Long Term Workforce Plan finds the total number of staff vacancies could grow to between 260,000 and 360,000 by 2036-37. The rising rate of obesity and its high cost are putting strain on the NHS because it heightens the risk of Type 2 diabetes, coronary heart disease, cancer and strokes.
Weight-loss drugs support the NHS because effective long-term weight loss should mean fewer heart attacks, fewer diabetes complications and fewer joint replacements, easing pressure and lowering the cost of obesity on the NHS. The Tony Blair Institute reported in May 2025 that weight-loss drugs could save the UK £52 billion by 2050. NHS England states, from June 2025, that Brits can get Mounjaro from primary care services if they have a BMI of 40 or more and live with four weight-related health problems. They can also get Wegovy if they have a BMI of 35 or more and if diet and exercise changes haven’t worked.
NICE has recommended that Mounjaro be prescribed for up to a possible 3.4 million Brits from March 2025, but due to financial pressures, the NHS has agreed to a staged rollout. It is estimated that 220,000 people will benefit in the first three years. By slowly expanding the injection to those who need it most, the NHS can control costs and prevent misuse of the drugs. It also helps minimise healthcare disparities and prevents just the affluent from having access to weight-loss drugs.
Despite their rollout on the NHS, research in the British Medical Journal highlights how stopping weight-loss drugs can have regressive effects, with many patients rapidly regaining weight once treatment ends. Research published in January 2026 finds that people who stopped taking weight-loss drugs return to their original weight and forgo any benefits gained within two years. These findings undermine the benefits of drugs like Wegovy and Mounjaro. For the NHS, this is likely to mean a rebound in obesity rates over the next five years, driving costs back up and piling extra pressure onto a service that’s already under strain. In the UK, the new NICE quality standard, from August 2025, recommends support for a year after the cessation of weight management drugs. However, research finds that this isn’t cost-effective, judging by the NICE threshold for cost-effectiveness.
Private rollout and widening health inequalities
It is estimated that 1.4 million Brits are accessing weight loss drugs privately, outside of the NHS, every month through private online pharmacies. Media hype and celebratory endorsements (like from Serena Williams, who used Zepbound for weight loss; however, she is also a paid ambassador for Ro, a telehealth GLP-1 provider) of weight-loss drugs are encouraging widespread use across the UK, as people are desperate to achieve the best body possible. This is leading to the creation of black markets for weight-loss drugs, unregulated products that can cause serious harm to individuals – for example, pancreatitis, gall bladder disorders and hypoglycaemia. In October 2025, the Medicines and Healthcare Products Regulatory Agency dismantled an illegal manufacturing facility in Northampton, where unlicensed weight-loss jabs were made and distributed. Without proper oversight, the weight-loss drug boom could do real harm, not least by fuelling dangerous black-market supply and misuse.
The use of privately bought weight loss drugs also exacerbates health care inequalities. These drugs aren’t cheap, with Eli Lily hiking the price of its popular drug Mounjaro in the UK by 170%, to £330 per month, in August 2025. Obesity is more prevalent in areas of deprivation in the UK. The Office for Health Improvement and Disparities (OHID) finds that in the UK, obesity prevalence is 37.4% in the most deprived decile. Parallel to this, demand for weight-loss drugs is highest among more typically disadvantaged groups.
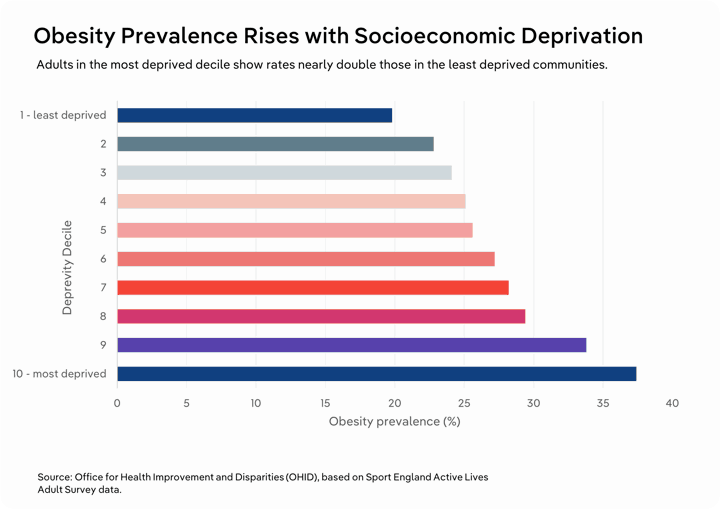
Poorer areas of the UK are also the least physically active, with the most deprived decile recording a 35.3% physical inactivity rate according to the OHID. Limited access to affordable, safe spaces for exercise makes it harder to be active, contributing to higher rates of obesity in deprived communities.Consumer confidence has remained weak through 2025-26 as inflation has stayed above the Bank of England’s 2% target and a rising tax burden has constrained growth in real household disposable income, keeping the GfK consumer confidence index in negative territory in January 2026. As household budgets remain tight, many people are likely to cut back on discretionary spending and focus on essentials, which will put costly weight-loss drugs out of reach for a large share of the population. By contrast, more affluent Brits will still be able to afford these treatments, meaning obesity rates and related risks like cardiovascular disease and Type 2 diabetes will fall fastest in this already advantaged group, widening health inequalities.
The economic benefits for the UK from investment in life sciences
The surge in demand for GLP-1 weight-loss drugs is transforming UK pharmacies and could boost the nation’s life sciences sector on the global stage. In October 2024, the government signed a landmark deal with Eli Lily, resulting in an £279 million investment into the UK. Although only in an agreement stage as of January 2026, the deal will boost the UK’s life sciences base and support new ways of tackling diseases, creating 300,000 jobs according to the Department of Health and Social Care in October 2024. The rapid growth of GLP-1 presents economic opportunities to create jobs, lift labour force participation by enabling those unable to work for health reasons to return to work, increase real consumer spending and help drive GDP growth.
Investment in UK life sciences is ever more important following Merck’s decision to scrap a £1 billion investment into a research centre in London in September 2025. Merck cited that the UK is an uncompetitive place to launch and sell new medicines, especially given how the NHS prices and funds drugs. According to the Association of the British Pharmaceutical Industry (ABPI), the UK is unattractive to invest in, falling down global rankings for pharmaceutical investment and research. It finds that high clawback rates on pharmaceutical companies revenues and poor clinical trial delivery dampen investor confidence.
By expanding access to modern weight-loss drugs, the UK aims to attract greater pharmaceutical investment, strengthen its life sciences sector, create new jobs and drive economic growth. However, ABPI argues that focusing on health data, AI and advanced therapies offers a more credible route to boosting life sciences investment, suggesting that relying on weight-loss drugs alone is an inadequate long-term growth strategy.
The effect of weight loss drugs on the food system
Weight-loss drugs work by suppressing appetite. People on weight-loss drugs typically reduce their calorie intake by 15% to 35%, cutting back on fatty or sweet foods. Weight-loss drugs have the ability to significantly shift demand within the food system in the UK. By shifting demand away from ultra-processed categories like sweets and snacks to nutrient-dense items like yoghurt and fresh produce, weight-loss drugs could create sustained change in consumer demand for healthier foods. Companies in the food industry are responding. Heston Blumenthal’s Fat Duck restaurant scaled down its tasting menu in September 2025 to meet growing demand for appetite-suppressing GLP-1s. Greggs is now offering smaller, higher-protein portions in response to the growth of weight-loss drugs.

Supermarkets are reporting shifts in consumer spending habits. Food categories like confectionery, crisps and alcohol are being hit the hardest, while demand for protein-enriched products (think yoghurt and cottage cheese) climbs. Supermarkets like M&S, Iceland and Ocado are focusing on meals with fewer calories and higher nutritional value, served in controlled, smaller portions, to target weight-loss drug users. Ocado has a new Weight Management aisle after research found that 73% of people said it would be helpful to know which meals can support lean muscle preservation when using GLP-1 drugs. Supermarkets need to adapt to shifting spending patterns as weight-loss drugs curb calorie intake and snacking; those that don’t risk weaker sales volumes and growing pressure on already thin margins.
Government initiatives like the salt reduction programme in the 2000s initially worked, but progress on sugar and calorie reduction has stalled. For example, despite Public Health England's 2024 Salt Reduction Targets to reduce salt in processed foods, sodium consumption hasn’t declined in the UK since 2014. Weight-loss drugs could catalyse a shift towards healthier diets, where the government has had little impact, reshaping consumer behaviour and driving greater demand for genuinely healthier products. However, weight-loss drugs alone aren’t enough and policy reform and regulatory change alongside them will support sustained change. For example, the recent healthy food standard introduced in June 2025 by the Department of Health and Social Care encourages producers and retailers to make products healthier.
The positive shift in consumer behaviour may be constrained by the nexus between the big food and big pharma industries. Research published by the Health Economics and Management Review in March 2025, finds that healthcare systems prioritise profit over prevention through regulatory capture, misleading nutritional guidelines and pharmaceutical dependency. It ensures continuous reliance on processed foods and medication. The pharmaceutical industry has monetised this through aggressive marketing of medication as the solution to a healthier lifestyle, shifting the focus away from dietary or lifestyle changes. This research underscores the possibility that consumer demand for unhealthy foods is a systematic issue that food and pharmaceutical companies profit from. This would dampen any possibility of weight loss drugs changing consumer behaviour in the long term.
Final Word
Weight-loss drugs aren’t the silver bullet. Although they can be used in the short term for significant weight loss, the long-term effects are that people often regain weight once they stop taking these drugs, nullifying the cost-saving benefits to the NHS. The ethical and public health concerns surrounding weight-loss drugs are valid and should be carefully considered alongside the potential economic opportunities.
Weight-loss drugs shouldn’t be used as a first port of call for tackling obesity and the social and environmental determinants must still be prioritised, especially by policymakers. However, with the introduction of weight loss pills in the UK around the corner, weight loss medication is likely to swell in popularity. Unless the NHS chooses to expand access to the drugs or regulation tightens, it will exacerbate concerns about a greater private-sector rollout, opening up the possibility of more black markets and worse health outcomes.